The fact that oral cancer is one of the few types of cancer that has not experienced a significant reduction in mortality over the past several decades is attracting more media attention and generating more public concern. Given that roughly two-thirds of oral cancers are discovered in late stages, when the five-year survival rate is only 50 percent, the key to reducing the devastating impact of this disease is earlier detection.
Many health experts cite the fact that the mortality rate of cervical cancer was reduced by 74 percent due largely to the impact of the Pap smear on early detection of that disease.
There is widespread agreement that dental practitioners are best suited to detect oral cancer. Virtually all dentists and hygienists are trained to conduct the conventional head and neck “white light” examination featuring palpation and visual inspection.
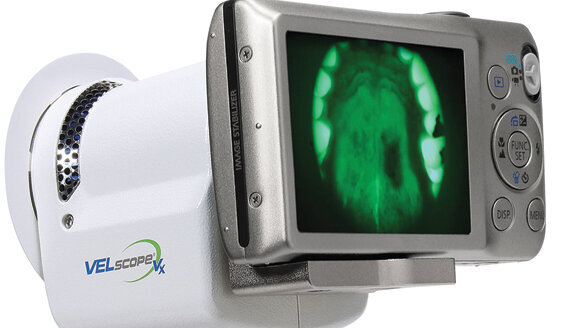
For several years, dental practices have also had the option of augmenting the “white light” examination with various adjunctive screening devices, including the VELscope tissue fluorescence visualization technology developed by LED Dental.
While thousands of practices have embraced this technology over the past five years and made it the world’s No. 1 oral mucosal screening device, others have opted to wait until more clinical evidence is available documenting the VELscope’s efficacy.
While several studies have been published supporting the VELscope’s value as an adjunctive screening device, a study recently published by Dr. Edmond Truelove and colleagues from the University of Washington provides perhaps the most impressive evidence yet of the VELscope’s efficacy. The article, “Narrow band (light) imaging of oral mucosa in routine dental patients. Part I: Assessment of value in detection of mucosal changes,” was published in the July/August issue of General Dentistry.
Background
The purpose of this investigation was to determine the value of adding the VELscope’s tissue fluorescence visualization examination to the standard oral soft-tissue examination used to detect mucosal change.
The study involved patients who visited the University of Washington clinic for regular dental evaluation or for treatment of acute dental problems. The 620 patients who chose to participate were of wide variety. Their ages ranged from 18 to 85; 55 percent were women; and 57 percent had a family history of cancer.
University of Washington dental students, while being supervised by faculty, gave patients routine head and neck physical examinations, followed by oral soft-tissue assessments and dental examinations under white light without any devices. They recorded their findings and then immediately examined patients again with the VELscope.
All areas shown by the VELscope examination to exhibit a loss of fluorescence — indicating tissue change — were recorded and classified clinically as normal variation, inflammatory, traumatic, dysplastic, or other. In addition, patients were categorized depending on their clinical findings: normal, need follow-up visit, or immediate biopsy.
Risk factors related to oral dysplasia also were recorded. The addition of the VELscope examination added between one and two minutes to the examination process.
Results
Of the 620 examinations, an area with loss of fluorescence suggestive of possible pathology was detected in 69 subjects (11.1 percent). After a second immediate evaluation, 28 of the 69 subjects were scheduled for follow-up or biopsy. The biopsies and follow-up appointments determined that two patients had lichen planus, two had inflammatory lesions, three had mild precancerous dysplasia and two had moderate precancerous dysplasia.
Importantly, none of the lesions discovered in these 28 subjects had been detected using standard “white light” examination.
Conclusions
The VELscope examination resulted in the detection of 28 lesions that would otherwise have gone undetected. Of these 28 patients, nine required further medical attention, and they received that medical attention because of the VELscope. The authors concluded that findings of the study support the use of the VELscope as “a simple adjunctive diagnostic device that, when used as one component of a standard diagnostic protocol, could help clinicians to detect inflammatory and dysplastic tissues.” They continued, “Use of this technology could improve clinicians’ ability to monitor and follow initially detected changes, and to better judge progression versus resolution and response to non-surgical treatments.”
Summary
VELscope technology has the potential to reveal oral cancer, precancerous dysplasia and other oral disease earlier than traditional white light exams. The earlier those oral abnormalities are caught, the greater the chance of patient survival and the less severe required treatment is likely to be.
When evaluating new technologies, it is virtually impossible to have 100 percent guaranteed proof of a product’s efficacy. For each new product, practitioners are forced to operate in a world of imperfect information and answer the question, “Is there enough clinical evidence that this technology really works?” In the case of the VELscope technology — and its latest generation model, the cordless VELscope Vx — it seems clear that a very strong case can be made that it in fact not only works, but that it can help reduce the impact of oral cancer, dysplasia and other oral disease.
(Source: LED Dental)
BURNABY, CANADA / NEW YORK, NY, USA: The World Health Organization (WHO) recently recognized the VELscope enhanced oral assessment system as an innovative ...
OTTAWA, Ontario, CANADA: The Canadian Dental Hygienists Association (CDHA) says that World Cancer Day (Feb. 4) is a perfect time for dental hygienists ...
TORONTO, Canada: Since the use of an antimicrobial oral rinse in intensive care units (ICUs) and its effectiveness in preventing pneumonia have been ...
An abnormal immune response or “feedback loop” could very well be the underlying cause of metastases in oral cancers, according to Dr. Marco ...
TORONTO, Ontario, CANADA: After examining data gathered over an 11-year period in a first-of-its-kind provincial study, University of Toronto ...
SASKATOON, Canada: Oral health can dramatically influence overall health and quality of life. This is especially true for those with developmental ...
NEW YORK, N.Y., USA: Robert S. Roda, DDS, MS, was installed as president of the American Association of Endodontists during AAE’s annual session, held...
LONDON, Canada: The use of artificial intelligence (AI) in dentistry is rapidly expanding, offering new possibilities in diagnostics, treatment planning and...
The concept of “value” has been defined as the worth of a good or service as determined by people’s preferences. And yet with dentists, ...
VANCOUVER, British Columbia: Perhaps nowhere at the Pacific Dental Conference do the event’s core offerings blend better than on the Exhibit ...
Live webinar
Mon. 8 June 2026
12:00 PM EST (Toronto)
Live webinar
Mon. 8 June 2026
1:00 PM EST (Toronto)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (Toronto)
Live webinar
Wed. 10 June 2026
11:00 AM EST (Toronto)
Live webinar
Wed. 10 June 2026
2:00 PM EST (Toronto)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 PM EST (Toronto)
Live webinar
Thu. 11 June 2026
1:00 PM EST (Toronto)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Latin America / Latinoamérica
Latin America / Latinoamérica
 USA / USA
USA / USA
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East











































To post a reply please login or register